
What is The Screen Project?

The Screen Project is a Canadian National initiative to make BRCA1 & BRCA2 screening available to all Canadians over 18 years of age at an accessible price. As part of The Screen Project, you will also help our team of researchers at the Familial Breast Cancer Research Unit of Women’s College Hospital evaluate the benefits of population-based genetic testing. We hope that our study will reduce the mortality from breast, ovarian, prostate and other cancers.
Breast cancer is the most common cancer among Canadian women and affects approximately 1 in 9 women. Ovarian cancer affects another 1-2% of women. Prostate cancer will affect about 1 in 7 men. We do not understand the cause of most cancers, but approximately 5-10% of all breast, ovarian and prostate cancers are hereditary and due to a mutation in a gene that is passed down from one generation to the next.
Mutations in two genes, BRCA1 and BRCA2, are strongly associated with breast, ovarian, and prostate cancers. Everyone has two copies of the BRCA1 and BRCA2 genes, which we inherit from each of our parents. Their function is to help prevent cancer in specific parts of the body. If the BRCA1 or BRCA2 gene is not working properly (due to genetic change or mutation), then there is an increased risk for cancer. BRCA mutations predispose women to a higher lifetime risk of breast (up to 80%) and ovarian cancer (up to 20 – 40%). Men with a BRCA mutation are at increased risk of developing prostate (up to 35%) and other cancers. It is estimated that one in every 300-400 Canadians carries a mutation in one of the two BRCA genes. However, members of certain groups are more likely to have a mutation than the average Canadian. These groups include:
- Women with a recent or past history of breast or ovarian cancer
- Men with prostate cancer (particularly metastatic and high risk, locally advanced prostate cancers)
- Men and women with pancreatic cancer
- Women and men with a family history of breast or ovarian cancer
- Individuals of Ashkenazi Jewish ancestry
Knowing if you have a gene mutation in BRCA1/2 (or another hereditary cancer gene) can help you and your doctor(s) better understand your risk of developing certain types of cancers. There are also screening/management options available to reduce the risk of developing cancer, detect cancer at an early stage, and identify more targeted treatments. It is also important information for your family members. In some cases, knowing this information can prevent cancer in relatives too.
Genetic testing through the Screen Project is based on a saliva sample that is provided to Invitae, our genetic testing partner (details about this process are available in the consent form). Your sample will initially be tested for the BRCA1 and BRCA2 genes. However, you will have the option to request additional testing once you receive your BRCA test results.
Typically, if someone decides to have genetic testing, you can get one of three types of results:
- Negative – this means the gene looks as it should (i.e. normal) and no changes or mutations were identified in the genes tested. However, this does not mean that you will never develop cancer. Cancer screening recommendations should still be based on your personal and family history.
- Positive – this means a significant, cancer-causing change (called a ‘pathogenic’ mutation) has been found in a gene, causing it to malfunction. This is believed to increase cancer risk in those who carry the mutation, however oftentimes screening/management recommendations are available.
- Variant of Uncertain Significance (VUS) – this means there is a variation (or difference) found in a gene, but it is not clear at this time whether this particular variation causes an increased risk of cancer in those who carry it, and if so, by how much. Keep in mind that we all carry minor genetic changes in our genetic information, therefore, most VUSes do not increase a person’s cancer risk. It is possible that over time a VUS may be ‘reclassified’, meaning that the genetics laboratory could have more information about the gene variant to know more confidently what it means (if anything). Typically, for people with a VUS result, their medical management is only based on their personal and family history and not on the presence of the uncertain gene variant.
If someone is found to carry a mutation in BRCA1, BRCA2 or another hereditary cancer gene (i.e. positive result), this may help explain why they got cancer or why they have a family history of cancer. This could also mean that they are at increased risk of developing cancer in the future. It is important to know that testing positive is not a diagnosis, and it does not mean a person will definitely get cancer.
Armed with this genetic information, gene mutation carriers can make informed decisions about how they would like to manage their increased risk for cancer. All participants found to carry mutations will speak with the study genetic counsellor to discuss their cancer risks and management options. Our team will also refer most newly identified gene mutation carriers to their local genetics clinic to further review the cancer risks, management options and for future follow-up.
If someone is found to carry a mutation in one of the genes, this can also have implications for family members. Any biological children or siblings (both male and female) will have a 50/50 chance of carrying the same genetic mutation and predisposition to cancer. Having a positive mutation result also likely means that one of person’s parents carries the same gene mutation, as may some of their relatives. Genetic testing is typically available to all adult, at-risk family members through a local genetics clinic.
To learn more about hereditary breast cancer and understanding the genetic testing results, you can watch the below short videos on YouTube:
Credit: Jewels in Genetics
Why Participate?
The benefits include receiving a genetic test that many Canadians are not eligible to receive through their provincial health care system. Furthermore, this genetic information may allow you to better manage your health and understand your risks for developing specific types of cancers.
Mutation carriers identified through the study will receive standard, one-on-one genetic counselling and will receive information about their cancer risk and the most current screening/management recommendations. They will also have access to long-term genetics care locally. Being identified as a gene mutation carrier may mean access to intensified screenings, taking medications to reduce cancer or preventative surgery that was not previously available. Family members may also benefit from having the explanation/cause of cancer in the family identified. Relatives would then also have the information to make more informed decisions about their health.
In addition, should you wish to have testing for additional genes (other than BRCA1 and BRCA2) related to hereditary cancers, this option is available through the Screen Project at no extra cost, after you receive your BRCA1 and BRCA2 genetic testing results.
It is also important to be aware that there are potential risks from participation in the study. The main risks are primarily of a psychological nature. For instance, those who receive a positive result and are at an increased risk of cancer, may feel a host of different emotions. However, getting a negative (uninformative) result can also leave people feeling uncertain and worried.
Genetic counselling will be provided to individuals who are identified as mutation carriers by our study genetic counsellor. Individuals who receive a negative or inconclusive result may also request genetic counselling from our study genetic counsellor or from genetic counsellor employed by Invitae.
There are also potential non-medical implications from your genetic test result. In the past, there had been concern about the impact of a positive genetic test result on future insurability and/or employability. As of May 4, 2017, the Genetic Non-Discrimination Act (GNA), formerly known as Bill S-201 was passed into law in Canada. This law protects individuals from the use of genetic test results for means of discrimination by potential or existing insurers. Under GNA, insurance providers cannot request or require that a person undergo genetic testing or disclose previous and/or future genetic test results in the clinical or research setting. However, GNA does not prohibit insurers from using information about pre-existing or previously diagnosed medical conditions. Family history is also not protected by GNA. Therefore, there may be circumstances that are not covered by the Act, as well as the rules and protections may be different in other countries.
Currently, genetic testing for hereditary cancers is offered through provincial programs, such as the Ontario Health. For individuals interested in genetic testing, they must meet specific criteria in order to qualify. This may include age at cancer diagnosis, ethnicity, and family history of breast or ovarian cancer. Typically, a patient is provided genetic counselling through a local cancer genetics clinic prior to proceeding with the genetic testing.
Currently, there are three major clinical gaps in identifying carriers of cancer predisposing BRCA1 and BRCA2 genes. Our goal is to address these gaps:
- Given the hereditary cancer testing eligibility criteria set out by provinces, access is limited to a small portion of the population (i.e. those with a strong personal or family history of cancer). Some individuals may carry a mutation yet do not qualify for genetic testing based on current guidelines. Additionally, some individuals who qualify for genetic testing fail to be identified and/or referred for genetic testing by their primary health care provider or specialist.
- Even if a person does meet testing eligibility criteria, hereditary cancer genetic testing is often offered to patients too late, with most tests done after a patient has been diagnosed with cancer. Our goal is to give people access to genetic testing before a diagnosis happens and use this information to hopefully prevent cancer or diagnose it at an earlier stage.
- Furthermore, in many cases, genetic testing is offered after cancer treatment has been completed. Ideally, knowing mutation status before or at the time of cancer diagnosis can help you and your medical team decide on the best course of treatment and/or surgery.
A long-term solution for addressing the clinical gaps outlined under the Current Model Tab is to have a national, population-based approach for hereditary cancer genetic testing. This approach uses genetic testing as a screening tool to identify high-risk patients, followed by genetic counselling to review and discuss the screening and prevention options available for those identified as high-risk. Genetic counselling resources would be directed toward the mutation carriers who need it the most. The two other main advantages of this model for genetic testing are that we can identify a larger proportion of mutation carriers in the population and more importantly, identify mutation carriers before they develop cancer so that they can be offered preventive/risk-reducing measures.
The Screen Project: A Population-Based BRCA Genetic Testing in Canada
Overall, a population-based approach gives all men and women the option of learning their BRCA1/2 and other hereditary cancer gene mutation status. As a result, they have an opportunity to make more informed decisions about their health. No studies have evaluated the cancer risks for mutation-carriers ascertained from the general Canadian population (patients unselected for their personal or family history of cancer). Therefore, before making recommendations for a nation-wide BRCA screening approach, it is important to assess the outcomes and level of interest in genetic testing among Canadians, and to determine the level of satisfaction among participants.
To do this, we have designed a prospective study named The Screen Project that will evaluate population-based genetic testing for hereditary cancer gene mutations in Canada. We hope that our research study may lead to accessible genetic testing for breast, ovarian, prostate and other cancers in Canada.
Genetic testing for cancer predisposition is now a standard component of clinical practice in oncology. Our main objective is to establish a Canada-wide population-based genetic testing model for BRCA and other hereditary cancer genes in order to identify as many mutation carriers as possible. Our ultimate goal is to reduce cancer morbidity and mortality from breast, ovarian, prostate and other cancers. For achieving that goal, The Screen Project has been designed with these five specific objectives in mind:
- To measure the feasibility of BRCA genetic testing among Canadian men and women using a guided direct-to-consumer approach
- To determine the frequency of BRCA1 and BRCA2 mutations in Canadians
- To evaluate the level of satisfaction among participants following a guided direct-to-consumer approach for BRCA genetic testing
- To measure levels of cancer-related worry among participants with a positive or negative genetic test result
- To estimate the number of breast, ovarian, and other cancers prevented in Canada through a guided direct-to-consumer approach for hereditary cancer genetic testing
We are group of researchers, consisting of Drs. Steven Narod, Mohammad Akbari, Joanne Kotsopoulos and Kelly Metcalfe. Angelina Tryon is the project’s genetic counsellor and research study coordinator. We are based at Familial Breast Cancer Research Unit, Women’s College Research Institute (WCRI), Women’s College Hospital (WCH), University of Toronto.
The Familial Breast Cancer Research Unit was established at Women’s College Hospital in 1995 and includes four core scientists, their trainees, and 30 support staff – all of whom are located at Women’s College Research Institute (WCRI). The team is led by Dr. Steven Narod and considered by many to be the world’s leading research team on management of hereditary breast cancer. The team has an international track record and many contributions to the field of hereditary breast and ovarian cancer. These scientific contributions have resulted in a better understanding of the implications of genetic susceptibility to cancer and have led to better outcomes among high-risk individuals. The team collaborates with scientists at 64 centres worldwide and has published more than 600 papers in the past 15 years.
The Screen Project is an initiative of Women’s College Hospital (WCH). To donate in support of women’s cancers research, care and education at WCH, please click here.
The Screen Project is an initiative of Women’s College Hospital (WCH). To donate in support of women’s cancers research, care and education at WCH, please click here.
Frequently Asked Questions
Our genes are the instructions for how our bodies develop and function. Over 20,000 genes have been identified in the human genome; we have 2 copies of each gene in every cell of our body (one gene copy is inherited from each of our parents).
The name “BRCA” is an abbreviation for “BReast CAncer.” BRCA genes include BRCA1 and BRCA2. Their function is to prevent DNA damage in cells in specific parts of the body. They are known as ‘tumour suppressor’ genes.
However, genetic mutations or changes to BRCA1 and BRCA2 genes have been found to impact a person’s chances of developing cancers such as breast, ovarian, prostate and other cancers.
Furthermore, in recent years many more genes have been discovered that when mutated, predispose an individual to breast, ovarian, prostate and/or other cancers (i.e. PALB2, ATM, CHEK2, etc).
No. These genes help prevent cancer in specific parts of the body. If a person’s BRCA1 or BRCA2 genes are not working properly (due to genetic change or mutation), then they are at an increased risk to develop cancer. It is not a guarantee that they will develop cancer; it just means that they are at elevated risk to develop certain cancers compared to the general population.
To find out if you have a BRCA gene mutation, you can choose to be tested through The Screen Project or your local genetics clinic if you meet provincial eligibility guidelines.
It is estimated that 1 in every 300-400 Canadians carries a BRCA1/2 gene mutation.
Mutations in other hereditary cancer genes are much less prevalent.
If you are female and have a BRCA1/2 gene mutation:
- You will have up to a 70% lifetime risk for breast cancer.
- You will have up to 20-40% lifetime risk for ovarian cancer.
If you are male and have a BRCA1/2 gene mutation:
- You will have up to a 35% lifetime risk for prostate cancer.
BRCA1/2 gene mutations can also be linked to an increased risk of developing other cancers as well.
Cancer risks associated with gene mutations in other hereditary cancer genes (i.e. PALB2, ATM, CHEK2, etc) can vary.
Identifying a mutation in a hereditary cancer gene may explain a person’s personal and/or family history of cancer. Mutation carriers may also benefit from specific cancer treatments tailored to their genetic makeup. This information may help a person reduce their risk of developing cancer. There are management options available, such as increased screening and surgical risk-reduction.
Yes. Some gene mutation-related cancers may still affect you regardless of your gender. An example is men with a BRCA mutation are at increased risk to develop prostate and male breast cancers. Early cancer screening is available for male BRCA mutation carriers.
Since this is a new model of cancer genetic testing provision in Canada, your participation will help us evaluate this way of reaching people and will also bring more awareness to hereditary cancer genetic testing.
The more people get tested for these mutations, the better our understanding will be of cancer gene mutation frequency and cancer risks associated with these gene mutations. The data gathered from this study will also help us to estimate the number of breast, ovarian and other cancers that can be prevented through population-based screening in Canada.
Genetic testing is a type of medical test that identifies changes in chromosomes, genes, or proteins derived from a DNA sample that you provide. The testing offered through the Screen Project specifically analyzes genes that are linked to hereditary cancer(s).
Genetic testing through the Screen Project is performed on a saliva sample that you provide. Details about this process are available in the consent form, and will also be provided to you after registration. The saliva sample that you provide will be tested for BRCA1/2 mutations.
Note: a blood sample is not necessary for genetic testing through the Screen Project.
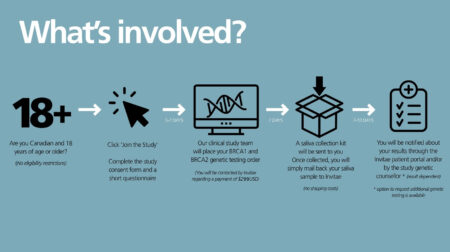
There are five steps involved in pursuing genetic testing through the Screen Project, each of them with different processing times:
- If you are a Canadian resident and 18 or older, complete the online study consent form & the short questionnaire.
- Our clinical study team will place your genetic testing order through Invitae, the genetic testing company. A saliva collection kit will be sent to your address from Invitae. You will be contacted by Invitae to pay a fee of $299 USD (approximately $350 – 400 CAD).
- You will mail back your saliva sample with the kit provided to Invitae.
- You will be notified about your results through the Invitae patient portal and/or by the study genetic counsellor. You will have the option of requesting additional analysis of 43 more genes at no additional cost.
It will take approximately two to three weeks to receive your results.
If you are a Canadian resident and over the age of 18, you are eligible to participate.
A negative genetic test result does not guarantee that you will be cancer free for the rest of your life. Still talk to your doctor about cancer screening based on your personal/family history.
You will have the option to request additional analysis of 43 more genes once you receive your BRCA1/2 test results, at no additional cost.
The following genes can be analyzed: APC, ATM, AXIN2, BAP1, BARD1, BMPR1A, BRIP1, CDH1, CDK4, CDKN2A, CHEK2, DICER1, EPCAM, FH, FLCN, GREM1, HOXB13, MEN1, MLH1, MSH2, MSH6, MUTYH, NBN, NF1, PALB2, PMS2, POLD1, POLE, PTEN, RAD50, RAD51C, RAD51D, RB1, RET, SDHB, SDHC, SDHD, SMAD4, STK11, TP53, TSC1, TSC2, and VHL.
The majority of hereditary cancer gene mutations are inherited in an autosomal dominant manner, which means one copy of the mutated gene is sufficient to increase a person’s chance of developing cancer. Any of your biological children or siblings (both male and female) will have a 50/50 chance of carrying the same genetic mutation and predisposition to cancer. Typically, one of your biological parents will carry the same gene mutation, as well as some of your relatives.
Yes, all participants will have to remit a fee of $299 USD directly to Invitae (our laboratory partner). This is to cover the cost of the test itself, and The Screen Project/Women’s College Hospital are not profiting off of this testing whatsoever. At this time, financial assistance is not available, however this may change in the future. Keep an eye on our website for updates.
You are welcome to reach out us via email at thescreenproject@wchospital.ca. Response times may vary, however we will try our best to respond to you within 2 – 3 business days.